The Infusion Company
Designed for the Future. Today.

All-in-One philosophy
One pump. All therapies.
Innovation
The core of our success.
The perfect solution for your hospital.
Our Innovations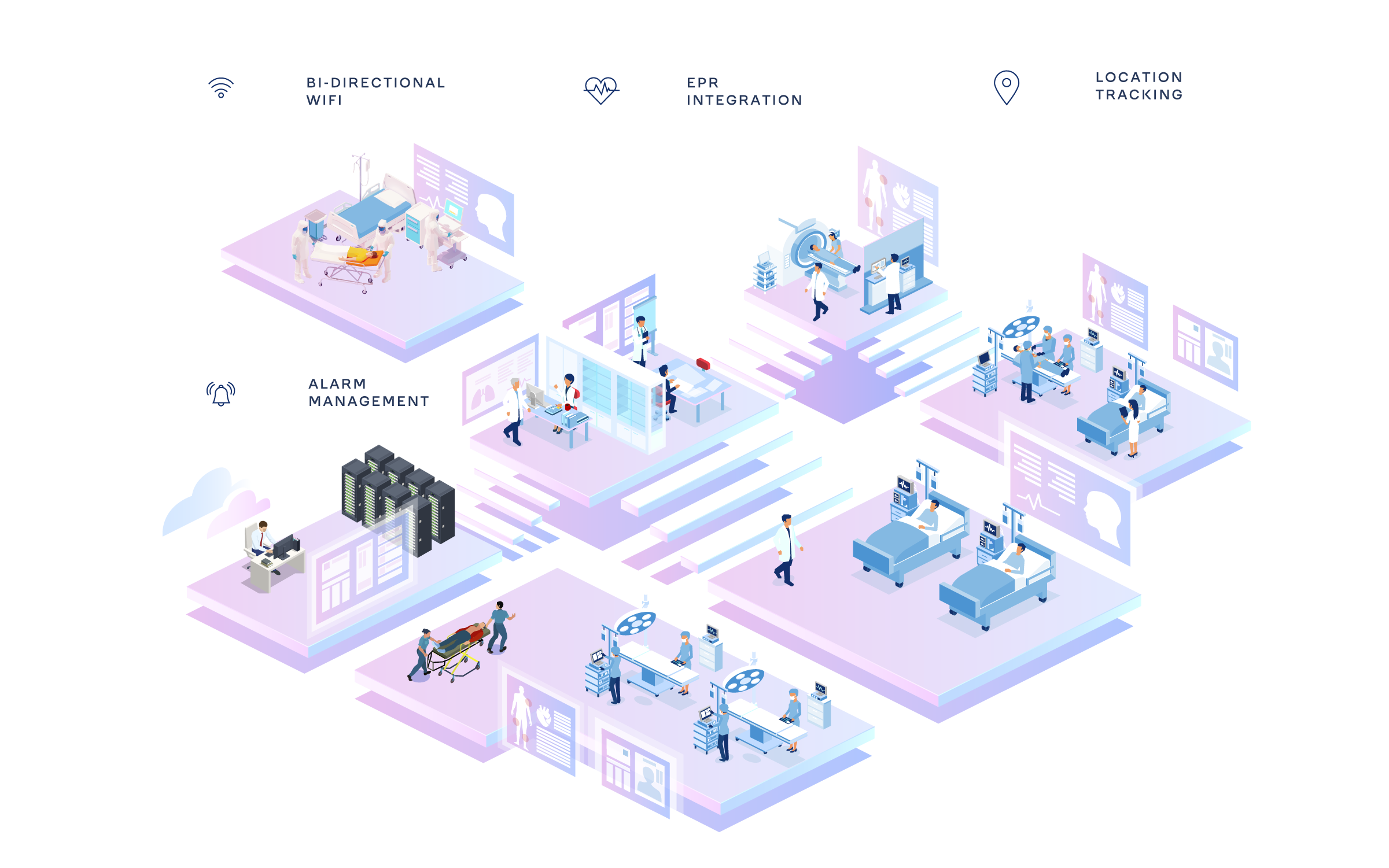
Reduce complexity. Increase safety.
Learn more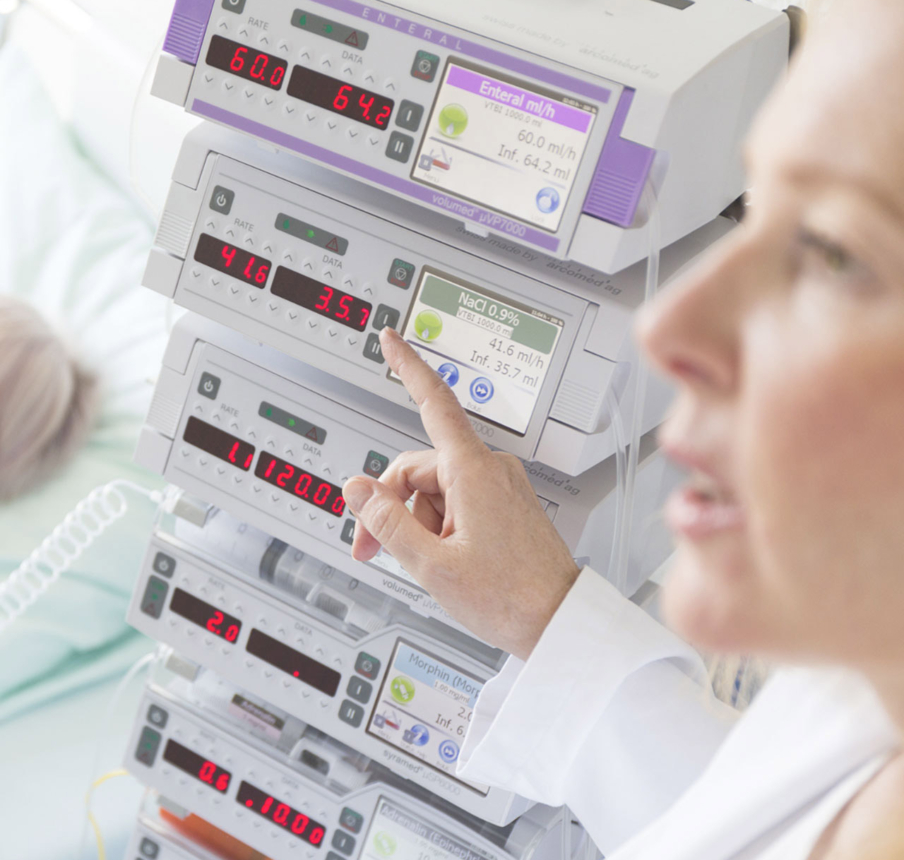
Most advanced anesthesia pump.
Learn more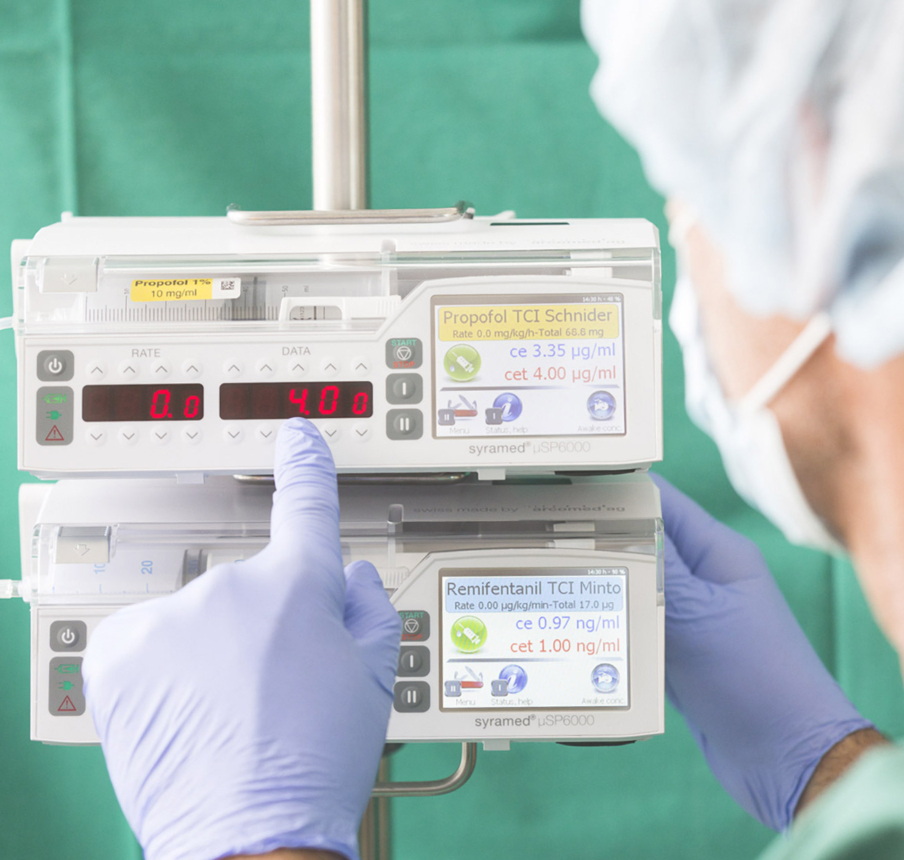
Pain simplified.
Learn more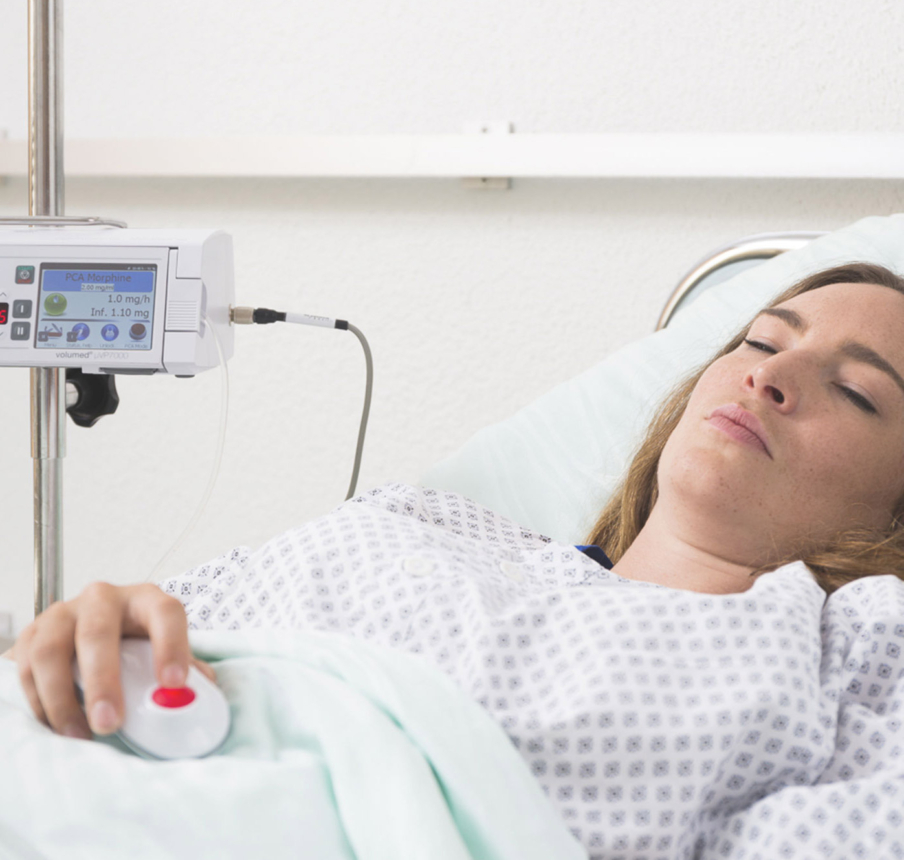
Maximise your safety.
Learn more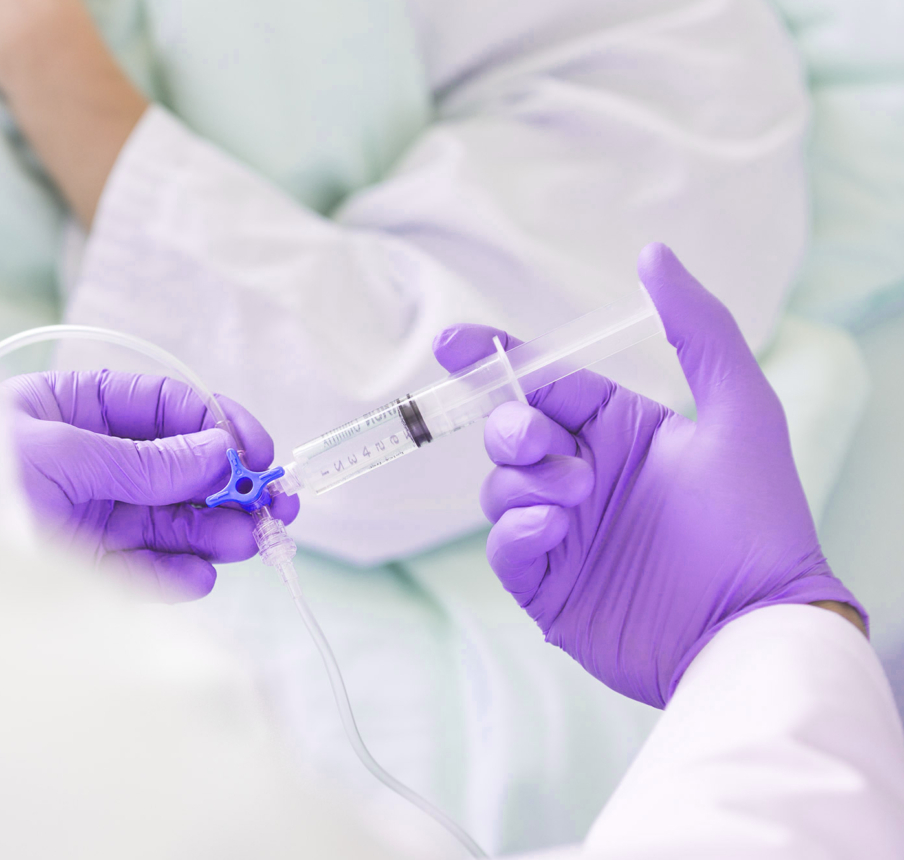
Simple safe solution.
Learn more
Certified hyperbaric therapy.
Learn more
Artifacts-free infusions.
Learn more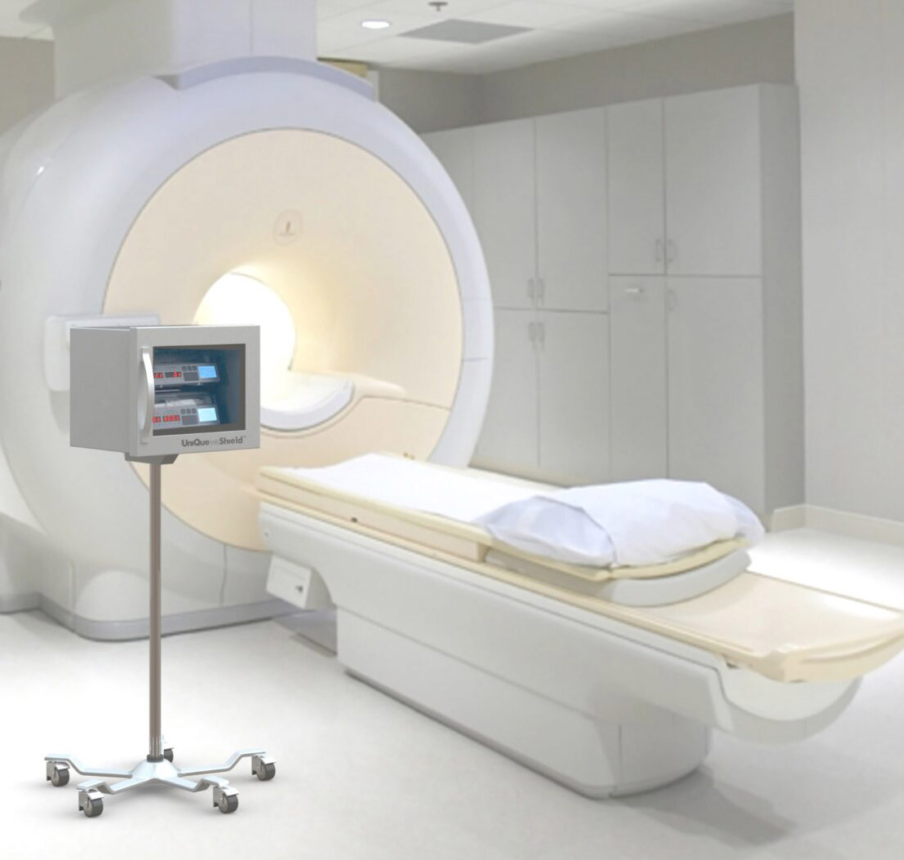
Where safety matters most.
Learn more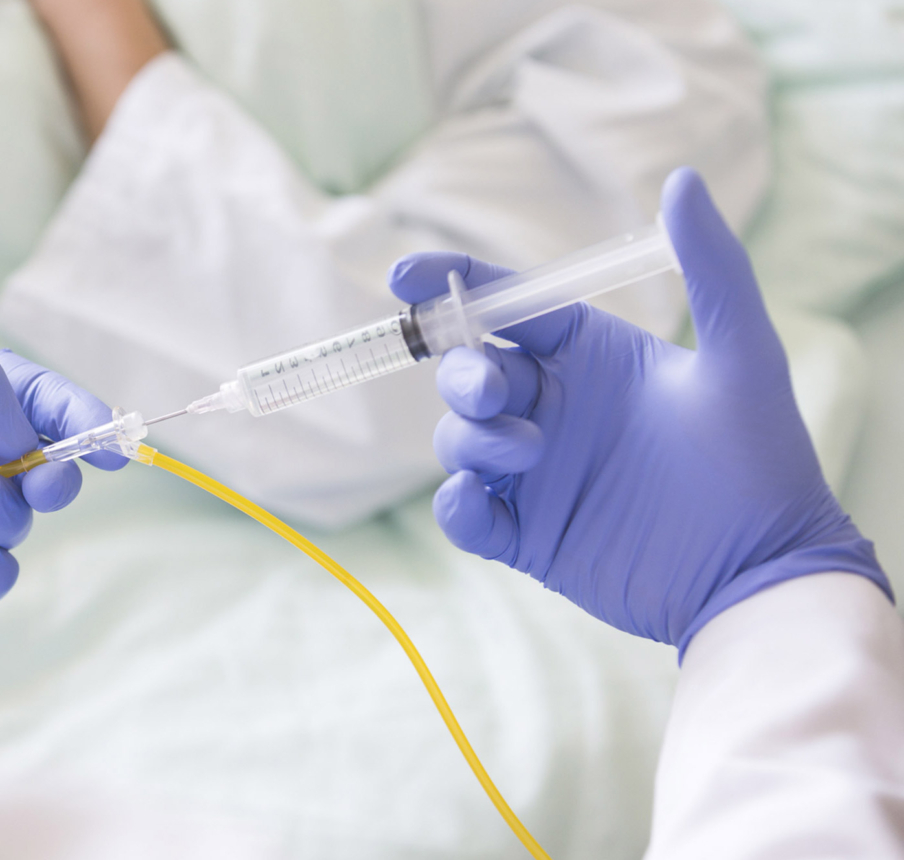
Integrated solution.
Learn more
Helping new beginnings.
Learn more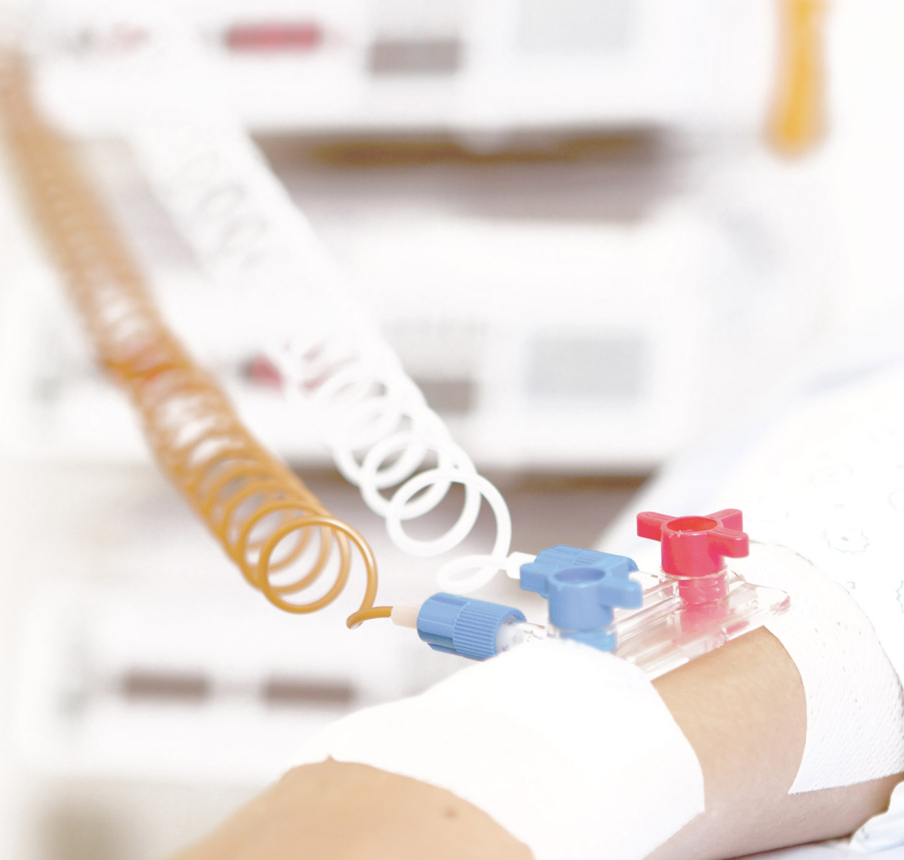

High-end Consumables.
Learn more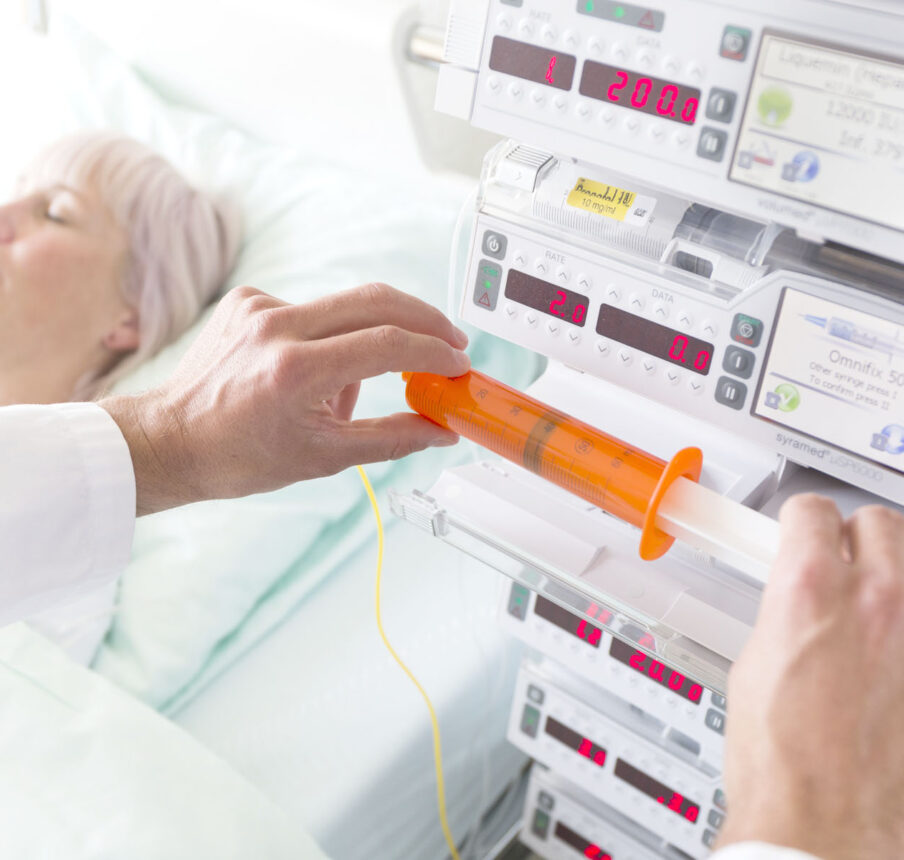
Less toxicity for patients and the environment.
Learn more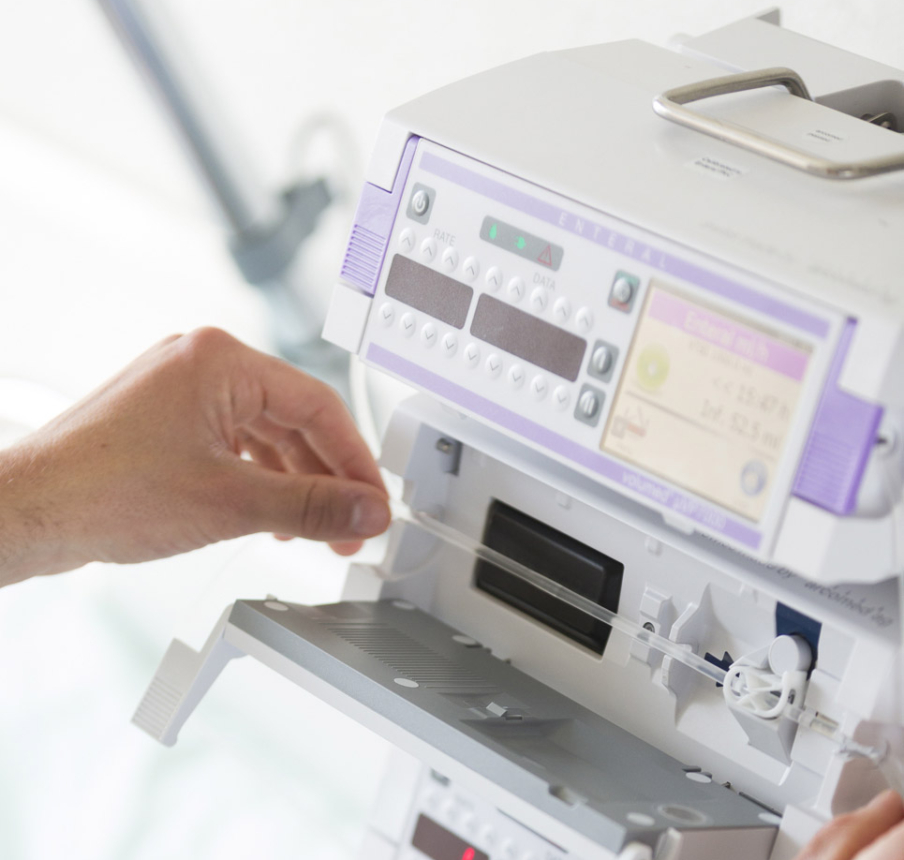
Wide range of syringe and extension lines.
Learn more
Extensive range of accessories.
Learn more